| My friend Wendy and I used to talk together a lot about food and our health, we found we had similar attitudes to our bodies and eating and were inclined to be on the rigid ‘this will be good for me’ side coming from our upbringing. In the year before she was diagnosed with bowel cancer Wendy became really committed to discerning a diet that she felt supported her body. |
She made every attempt to listen to the body's symptoms and feel how her body was responding to various foods. She thought she had Irritable Bowel Syndrome and we often talked about the energetic/psychological/emotional source of this. I remember the quite cosy times we used to have together encouraging each other. Then one day she told me she had been diagnosed with terminal cancer and that death could be very quick.
Everything changed, it seemed like she snapped into action, fully committed to preparing herself for this journey. She knew just what she wanted, just what she felt to eat, and just what she felt was needed.
The whole dynamic of our relationship was changed. I had to be very careful not to drop into any sort of sympathy, she did not need that, and I felt she was presenting something quite hard and definite to prevent others falling into that mode. I honestly did not feel sympathy and felt I wasn’t expressing it, but in a way, I did not feel open to her or embrace her in the same way that I had before.
The first time she went into hospital I went to visit her and take her some lunch, providing carefully what she had asked for. Utmost respect of her wishes and how she had chosen to be was so important.
We had a fun time together, light, playful, beautiful. But near the end of the visit I felt something else was needed, we were skating along on the surface, and her legs, being swollen to twice their size, were giving her huge pain. I suggested some gentle massage of her knees, the most painful place and where I could reach. She agreed with alacrity, but we began by going into it in the same energy we had been talking with.
I suggested we pause and take some gentle breaths. So, we did, and as we gently breathed the ward fell quiet, a stillness descended on everyone, nurses moved around gently, and I felt the Masters come in. Then I massaged her legs and gradually the pain receded, her face pinked up, and she was quieter.
I then left her and was aware that a ‘Magic of God’ moment had happened.
My next visit was an overnight at her home. This was very different. By now Wendy had chosen not to eat, she was in bed except for her toileting, and very weak and her pain managed by morphine. She still knew just what she wanted, where things needed to be placed, when to sleep, when to speak, who she wanted to speak to, how much she wanted to share her condition or talk of other things. All this needed to be respected.
It is a difficult transition between the time of the old friendship with its many habits and patterns, and this new relationship where there is so much to be learned about how to be with someone who is approaching the end of their life rapidly.
The patient is going through a transformation that the carer cannot fully understand as we have never experienced it, only second hand. I found the most important and hardest thing was to get myself out of the way, and to follow Wendy’s lead.
Maybe it could have been more like this in our relationship before her diagnosis – listening without reacting, not bringing an agenda about what we thought or believed, not imposing ourselves on the other person, not chatting away about totally unnecessary subjects, honouring and respecting who the other really is and meeting in that place. That would have prepared us both for this time.
I fell into the trap of having an agenda, as I had previously nursed my husband through terminal cancer. “Ah!” I thought, “An opportunity to re-imprint where I know I let us both down before.” But no, I knew as soon as I expressed this in a message to the very experienced palliative care nurse Elizabeth, that what I felt and said was completely about ‘me’, and did not belong at the bedside of someone preparing to die, and later Elizabeth confirmed that.
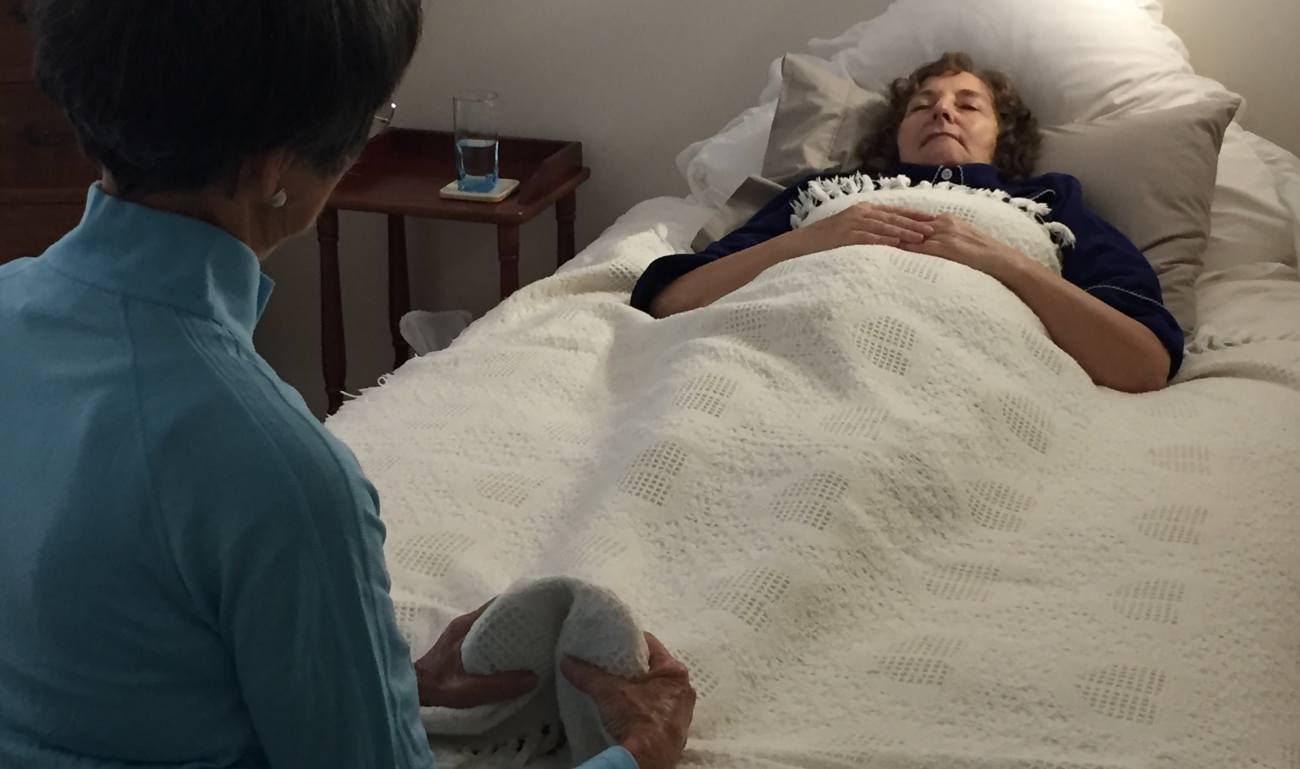
When I first entered the house, Elizabeth was sitting at the end of Wendy’s bed with her hands on her feet. She was very still, just being and holding, fully focused and present as a loving energy flowed from her; I could feel it, the stillness, the space, the love, and it filled the whole house.
There has to be purpose; a purpose that would serve both Wendy and the whole of humanity, for each loving and fully well-lived death contributes to an increased and expanding understanding and consciousness of how death can be, rather than the fear of death and dying which is so prevalent in today’s society.
There is also a purpose in caring for the patient with the utmost love and tenderness and support. A carer cannot bring any of their own emotions or ideals and beliefs into the room, it will hold the patient back.
Anxiety gets in the way. I have to own up to being anxious, which means I could not be wholly with myself, and I could feel how that anxiousness is about me, and is an emotion Wendy could have done without. But I did have tools to bring me back to myself and connect to my heart. I know I was in a mixture of in and out of confidence. I am not the world’s most practical person, and the need to be centred and calm and quiet inside was possible if I paid attention to how I moved in the room and lifted things and handed things to Wendy and her daughter.
To be a true carer it must be so lived in you that it is natural. All I can say is that I was willing to be there for my friend, that I did my best, and most important I was aware of what was going on and could make choices to change my energy of approach. I allowed myself to just observe and really get out of the way when Wendy and her daughter were together, and also to support her daughter when we were together. We shared a meal and she was able to speak some of her feelings.
I only did that one night shift, and am thankful for the opportunity to support my friend.
I could feel in Wendy’s dying the common experience for us all, the cycle of birth and death, the bigger picture of us all as a human brotherhood as we go from birth to death, and then back to do it all again. We are all together, connected.
Joan C., UK
Everything changed, it seemed like she snapped into action, fully committed to preparing herself for this journey. She knew just what she wanted, just what she felt to eat, and just what she felt was needed.
The whole dynamic of our relationship was changed. I had to be very careful not to drop into any sort of sympathy, she did not need that, and I felt she was presenting something quite hard and definite to prevent others falling into that mode. I honestly did not feel sympathy and felt I wasn’t expressing it, but in a way, I did not feel open to her or embrace her in the same way that I had before.
The first time she went into hospital I went to visit her and take her some lunch, providing carefully what she had asked for. Utmost respect of her wishes and how she had chosen to be was so important.
We had a fun time together, light, playful, beautiful. But near the end of the visit I felt something else was needed, we were skating along on the surface, and her legs, being swollen to twice their size, were giving her huge pain. I suggested some gentle massage of her knees, the most painful place and where I could reach. She agreed with alacrity, but we began by going into it in the same energy we had been talking with.
I suggested we pause and take some gentle breaths. So, we did, and as we gently breathed the ward fell quiet, a stillness descended on everyone, nurses moved around gently, and I felt the Masters come in. Then I massaged her legs and gradually the pain receded, her face pinked up, and she was quieter.
I then left her and was aware that a ‘Magic of God’ moment had happened.
My next visit was an overnight at her home. This was very different. By now Wendy had chosen not to eat, she was in bed except for her toileting, and very weak and her pain managed by morphine. She still knew just what she wanted, where things needed to be placed, when to sleep, when to speak, who she wanted to speak to, how much she wanted to share her condition or talk of other things. All this needed to be respected.
It is a difficult transition between the time of the old friendship with its many habits and patterns, and this new relationship where there is so much to be learned about how to be with someone who is approaching the end of their life rapidly.
The patient is going through a transformation that the carer cannot fully understand as we have never experienced it, only second hand. I found the most important and hardest thing was to get myself out of the way, and to follow Wendy’s lead.
Maybe it could have been more like this in our relationship before her diagnosis – listening without reacting, not bringing an agenda about what we thought or believed, not imposing ourselves on the other person, not chatting away about totally unnecessary subjects, honouring and respecting who the other really is and meeting in that place. That would have prepared us both for this time.
I fell into the trap of having an agenda, as I had previously nursed my husband through terminal cancer. “Ah!” I thought, “An opportunity to re-imprint where I know I let us both down before.” But no, I knew as soon as I expressed this in a message to the very experienced palliative care nurse Elizabeth, that what I felt and said was completely about ‘me’, and did not belong at the bedside of someone preparing to die, and later Elizabeth confirmed that.
When I first entered the house, Elizabeth was sitting at the end of Wendy’s bed with her hands on her feet. She was very still, just being and holding, fully focused and present as a loving energy flowed from her; I could feel it, the stillness, the space, the love, and it filled the whole house.
There has to be purpose; a purpose that would serve both Wendy and the whole of humanity, for each loving and fully well-lived death contributes to an increased and expanding understanding and consciousness of how death can be, rather than the fear of death and dying which is so prevalent in today’s society.
There is also a purpose in caring for the patient with the utmost love and tenderness and support. A carer cannot bring any of their own emotions or ideals and beliefs into the room, it will hold the patient back.
Anxiety gets in the way. I have to own up to being anxious, which means I could not be wholly with myself, and I could feel how that anxiousness is about me, and is an emotion Wendy could have done without. But I did have tools to bring me back to myself and connect to my heart. I know I was in a mixture of in and out of confidence. I am not the world’s most practical person, and the need to be centred and calm and quiet inside was possible if I paid attention to how I moved in the room and lifted things and handed things to Wendy and her daughter.
To be a true carer it must be so lived in you that it is natural. All I can say is that I was willing to be there for my friend, that I did my best, and most important I was aware of what was going on and could make choices to change my energy of approach. I allowed myself to just observe and really get out of the way when Wendy and her daughter were together, and also to support her daughter when we were together. We shared a meal and she was able to speak some of her feelings.
I only did that one night shift, and am thankful for the opportunity to support my friend.
I could feel in Wendy’s dying the common experience for us all, the cycle of birth and death, the bigger picture of us all as a human brotherhood as we go from birth to death, and then back to do it all again. We are all together, connected.
Joan C., UK